Background
Nail-patella syndrome (NPS; OMIM 161200) is an autosomal dominant condition characterized by the classical clinical tetrad of nail dysplasia, patellar aplasia-hypoplasia, elbow arthrodysplasia, and iliac horns. The nails may be absent, hypoplastic, or dystrophic with ridges, pits, and/or triangular lunulae.
See the image below.
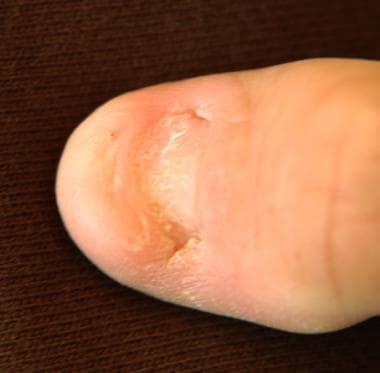
Nail of a patient the nail-patella syndrome.
Typically, nail anomalies are symmetric; the thumbs are most severely affected, and severity decreases progressing toward the fifth digit. The patella may be absent, small, or irregularly shaped. Dislocation in a superior and lateral direction is common if patellae are present. Elbow anomalies may include decreased extension, pronation, supination, and/or pterygia. Patellae and elbow anomalies may be asymmetric. The iliac horns are bony prominences that project posterolaterally from the iliac bones. Although rarely palpable, they are radiographically visible in most patients with nail-patella syndrome.
Proteinuria with or without hematuria occurs in 30-50% of affected individuals, but progresses to end-stage renal disease in approximately 5% of patients.
Ocular hypertension and open-angle glaucoma is more common in younger patients than in the general population.
The third documented chromosomal linkage identified in humans was between the nail-patella syndrome locus and the ABO blood group on chromosome 9.
LMX1B, located at 9q34.1, is an LIM-homeodomain transcription factor required for the normal development of dorsal limb structures, the glomerular basement membrane, the anterior segment of the eye, and dopaminergic and serotonergic neurons. Heterozygous loss-of-function mutations in LMX1B cause nail-patella syndrome.