Practice Essentials
Neuropathic arthropathy (Charcot joint) can be defined as bone and joint changes that occur secondary to loss of sensation and is most often associated with diabetes,
syphilis, syringomyelia,
spina bifida, traumatic spinal cord injury,
and leprosy.
The radiographic changes of this condition include destruction of articular surfaces, opaque subchondral bones, joint debris, deformity, and dislocation (see the images below). Neuropathic arthropathy (Charcot joint) poses a special problem in imaging when it is associated with a soft-tissue infection.
Leprosy is one of many causes of neuropathic arthropathy; joint manifestations of this disease include signs of Charcot disease, which advances despite treatment. Neuropathic arthropathy related to diabetes, syphilis, leprosy, and connective tissue disorders is more common in the elderly population. Neuroarthropathy related to asymbolia, spina bifida, and spinal trauma is more common in young individuals. Sensory impairment associated with spina bifida and myelomeningocele is the most frequent cause of neuropathic arthropathy (Charcot joint) in childhood.
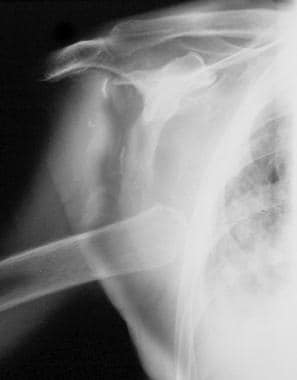
Neuropathic arthropathy (Charcot joint). Neuropathic arthropathy of the shoulder in a patient with syringomyelia. Note the destruction of the articular surface, dislocation, and debris, which are pathognomonic for a neuropathic joint.
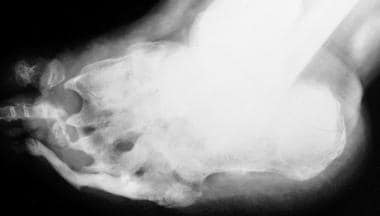
Neuropathic arthropathy (Charcot joint). Osteolysis of the distal metatarsals and phalanges with tapering results in a pencil-like appearance in the late stage of diabetic neuropathy.
Charcot arthropathy can occur at any joint; however, it occurs most commonly in the lower extremity, at the foot and ankle in patients with diabetes. It is seen in up to 9% of patients with diabetic neuropathy.
Similar pathology can also occur in the knee but is much less common and should be considered in a patient with peripheral neuropathy, who presents with a red, hot, tender, and swollen knee joint.
Syringomyelia is the main cause of upper extremity Charcot arthropathy, most often in the shoulder, although wrist and interphalangeal joint involvement have also been reported.
Charcot spinal arthropathy (CSA), also called spinal neuroarthropathy, is a rare mechanical destructive process that affects the intervertebral disc and adjacent vertebral bodies in patients who have loss of joint protective mechanisms.
Neuropathic arthropathy can be classified into hypertrophic and atrophic types. Hypertrophic changes predominate in the upper motor neuron lesions, and atrophic changes occur in peripheral nerve injuries. The early stage of osteoarthritis simulates neuropathic arthropathy, both radiologically and pathologically.
Progressive joint effusion, fracture, fragmentation, and subluxation should raise the suspicion of neuroarthropathy. In the advanced stage, abnormal findings on radiographs include subchondral sclerosis, osteophytosis, subluxation, and soft-tissue swelling. Long-standing neuroarthropathy is characterized by disorganization of joints. The finding of considerable amounts of cartilaginous and osseous debris within the synovial membrane (termed detritic synovitis) should alert the pathologist that the changes may represent a neuropathic joint. Other causes of detritic synovitis include osteonecrosis, calcium pyrophosphate dihydrate crystal deposition disease, psoriatic arthritis, osteoarthritis, and osteolysis with detritic synovitis.
Preferred examination
Radiography may be the only imaging required for the diagnosis of neuropathic arthropathy (Charcot joint). In the appropriate clinical setting, a fairly accurate diagnosis can be achieved. The role of magnetic resonance imaging (MRI) and radionuclide scanning is to differentiate soft-tissue infection from osteomyelitis.
An indium-111 WBC scan often is used because it is more specific than the technetium-99m scan.
Radiographic findings in the early stages of neuropathic arthropathy (Charcot joint) may simulate osteoarthritis. Radiographs may not demonstrate findings that help in diagnosing osteomyelitis in neuropathic joints, which is a common problem.
The roles of ultrasonography and CT scanning are limited. Ultrasonography can be used to identify any local collection when infection occurs and to guide aspiration for cytologic analysis; however, it provides no further information regarding the integrity of underlying bone. Although CT scanning may be helpful in evaluating cortical destruction, sequestra, and intraosseous gas, these changes are not specific for neuropathic arthropathy.
Bone marrow edema is nonspecific and has several causes; therefore, differentiating bone marrow edema from neuropathic arthropathy (Charcot joint) may not be possible on the basis of MRI findings alone. Similarly, enhanced bone activity on radionuclide scans is a nonspecific finding and may occur with several neoplastic, inflammatory, and degenerative processes.
Differential diagnosis and other problems to be considered
Calcium pyrophosphate deposition disease and primary osteoarthritis are in the differential diagnosis. In addition, in the early stage, neuropathic arthropathy (Charcot joint) can simulate osteoarthritis, and bone fragmentation and collapse are seen in osteonecrosis, posttraumatic osteoarthritis, intra-articular steroid injection, infection, and alkaptonuria.
Baker et al reviewed neuropathic arthropathy in diabetics.
Neuropathic diabetic arthropathy, particularly in the feet, is the leading cause of morbidity in diabetic patients. It has many mimics. Ulcers, sinus tracts, or an abscess with an adjacent region of abnormal signal intensity in bone marrow suggests osteomyelitis. Contrast-enhanced MRI allows differentiation of viable tissue from necrotic regions in diabetic foot infections, which require surgical debridement in addition to antibiotic therapy. Subtraction images are particularly useful for visualizing nonviable tissue.
Dialysis-associated spondyloarthropathy occurs in diabetic patients with a long history of hemodialysis. Intervertebral disk space narrowing without T2 signal hyperintensity, extensive endplate erosions without endplate remodelling, and facet joint involvement are suggestive of spondyloarthropathy instead of infectious discitis or degenerative disc disease. The clinical features of infective discitis and spondyloarthropathy overlap, but knowledge of the patient’s medical history, as well as recognition of imaging characteristics described above, allows the radiologist to make a prompt and accurate diagnosis, leading to appropriate treatment.
Guidelines
The National Institute for Health and Care Excellence (NICE) of the United Kingdom has published a guideline for the prevention and management of diabetic foot disorders. Recommendations specifically relevant to Charcot arthropathy in diabetes are as follows
:
If a person with diabetes fractures a foot or ankle, the fracture may progress to Charcot arthropathy.
Acute Charcot arthropathy should be suspected if redness, warmth, swelling, or deformity (particularly if the skin is intact) is noted, especially in the presence of peripheral neuropathy or renal failure. Acute Charcot arthropathy should be considered even when deformity is not present or pain is not reported.
If acute Charcot arthropathy is suspected, a weightbearing radiograph of the affected foot and ankle should be obtained. Magnetic resonance imaging (MRI) may be considered if the radiograph is normal but Charcot arthropathy is still suspected.
The 2017 International Diabetic Foundation (IDF) guidelines on the diagnois and management of the diabetic foot also address Charcot arthropathy and include the following recommendations
:
In all patients presenting with a new diabetic foot infection (DFI), serial plain radiographs of the affected foot should be obtained to identify bone abnormalities (deformity, destruction) as well as soft-tissue gas and radiopaque foreign bodies.
Serial radiographs should be used to reassess potential osseous changes when healing progresses slowly or signs and/or symptoms worsen.
For patients who require additional imaging, particularly when soft-tissue abscess is suspected or the diagnosis of osteomyelitis remains uncertain, MRI is the study of choice.
In the acute phase, Charcot arthropathy may appear clinically similar to osteomyelitis. MRI findings consistent with an infection generally include soft-tissue fluid collection, sinus tracts, and diffuse marrow edema.