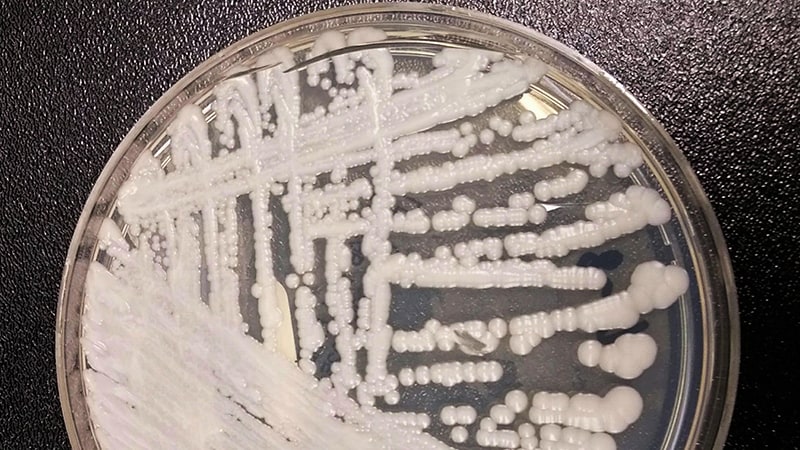
RECIFE, Brazil — The Brazilian National Health Surveillance Agency (Anvisa) recently reported a Candida auris outbreak in the northeastern state of Pernambuco. This follows two previously reported genetically connected outbreaks in the state of Bahia that occurred 1 year apart. Genetic testing is still ongoing, but it is presumed that the outbreak in Pernambuco is not connected to the other outbreaks.
In the case of suspected C auris colonization, physicians must isolate the patient, take the necessary precautions (similar to the precautions taken in cases of multidrug-resistant bacteria), and actively search for other cases.
In addition to sounding the alarm for the associated hospital infection control commissions, other regulatory bodies and institutions must be notified immediately, including Anvisa, the State Department of Health, the State Office for Infection Prevention and Control, the Center for Strategic Information on Health Surveillance, the applied epidemiology program of the Services of the Unified Health System (EpiSUS), the Public Health Central Laboratories (LACENs), the Public Health Laboratories General Office, and the Special Mycology Laboratory/Unifesp.
Why Such Concern?
The report published by Anvisa states that “studies indicate that up to 90% of Candida auris isolates are resistant to fluconazole, amphotericin B, or echinocandins,” and that the microorganism “can persist in the environment for prolonged periods (weeks or months) and shows resistance to several disinfectants.” In addition, “the difficulty in identifying the pathogen in a timely manner using standard laboratory methods and the difficulty in eliminating it from the contaminated environment” means that outbreaks can easily occur. The agency also reports that the fungus “can cause bloodstream infections and other invasive infections, which can be fatal, especially for patients who are immunosuppressed or who have comorbidities.”
Medscape’s Portuguese Edition spoke to three specialists about what the medical community needs to know about this emerging pathogen that poses a serious public health threat: Filipe Prohaska, MD, from the University of Pernambuco, who is a member of the team that identified the outbreak in Pernambuco; João Nóbrega de Almeida Júnior, MD, PhD, from the Special Mycology Laboratory of the State of São Paulo School of Medicine of the Federal University of São Paulo, who participated in the research involving the outbreaks in Bahia; and Flávio de Queiroz Telles, MD, infectious diseases specialist and director of the mycology committee of the Brazilian Society of Infectious Diseases.
C auris “is a fungus that occurs in hospitals and behaves like bacteria,” with infection being transmitted from one patient to another, said Telles, who is also a professor of infectious diseases at the Federal University of Paraná. Although “there is still no technical information on the drug resistance of the Brazilian C auris isolates, it is concerning because it can become multidrug-resistant,” he added.
Until now, cases have been identified in only two cities — Salvador in Bahia, and Recife in Pernambuco — but clinicians need to be aware that the fungus exists, and “that it is different from other species because it is highly resistant, and because it persists in the hospital environment,” Telles explained.
“It is a fungus that is impossible to eliminate when it enters an environment and colonizes it,” added Prohaska, who is also a mycologist at the Oncoclínicas Group. Alcohol-based products are still the standard method for sanitization, “but they have proven to be insufficient,” he said. The three specialists agree that there is not enough scientific evidence to support any alternative methods of sanitization. Ultraviolet B radiation has been able to eliminate the microorganism in experimental studies, but the exposure time has not been well studied, and protocols have not yet been established.
Almeida Júnior, who is also an attending physician at the Albert Einstein Israeli Hospital laboratory, recommended other methods but recognized that these are not always available.
“In the United Kingdom, hydrogen peroxide steamers are often used in patient rooms. We don’t have them here, but there are hydrogen-peroxide-based products on the market. Sites with fewer resources can use products that contain 0.1% sodium hypochlorite. The use of individual rooms and the availability of nursing assistants to care exclusively for C auris–colonized patients helps, but this is difficult to implement in a public hospital. Water, soap, and alcohol to clean hands are also important in preventing horizontal transmission,” he said.
Resistance to Antifungal Agents
The possible lack of treatment is also concerning. “Unfortunately, the vast majority of isolates are resistant to the antifungal agents available on today’s market,” said Prohaska. “In an attempt to minimize proliferation,” clinicians have been combining antifungal agents. But, he added, “the most important measures are to remove tracheostomy tubes and central venous catheters and reduce risk factors, such as corticosteroid and immunosuppressant use, to see if better results can be obtained by improving the patient’s immunity and reducing invasiveness.”
According to Almeida Júnior, resistance to echinocandin is still rare in Brazil, and it is the antifungal agent of choice for all severe forms of candidiasis. However, Telles cautioned that it does not penetrate the urinary tract very well, which means that if physicians use it for patients with C auris candiduria, they could be contributing to increased resistance.
The future of treatment does not seem very promising. Daniel Clemente de Moraes, a pharmacist from the Estácio de Sá University, conducted an integrative review on the current situation in the search for new antifungal agents that can be used to treat patients with C auris infections. The results, published in the Journal of Medical Mycology, indicate that, of 101 substances, two are under investigation in phase 3 clinical trials: ibrexafungerp and rezafungin.
The review clarifies main limitations of the research: few studies assessed the in vivo activity or the mechanism of action of the substances. According to de Moraes, this information is essential to ensure the lack of toxicity of a drug candidate. Moreover, knowing the mechanism of action can help predict antifungal resistance. As such, even if these substances are approved, they must be used with caution to reduce the possibility of the fungus developing resistance, which is the greatest challenge faced in antimicrobial discovery.
Diagnostic Difficulties
Specialists have also pointed out issues related to diagnosis. According to Prohaska, due to limited knowledge of the disease, a lack of orders to isolate fungal cultures, and — most important — insufficient diagnostic methods available to health services, the infection is still most likely highly underdiagnosed.
“Perhaps the outbreak has been ongoing, and we are only now able to diagnose it,” he said. “Several cities still use rudimentary methods and it is likely that they will not have been able to make the diagnosis.”
In addition, when doctors order a bacterial culture, they must add a fungal culture, he said, even though some automated methods cannot identify C auris. “Candida guilliermondii and Candida haemulonii are two species that, if detected in the hospital, must be sent to the central laboratories of the referring hospitals to confirm that they are not actually C auris,” said Prohaska.
Telles agrees that the problem could well be underestimated, given the challenges of diagnosis. “The health authorities feared some laboratories would be unable to identify C auris; this was highly emphasized before the pandemic. The warning was passed on to all the hospitals, and several LACENs were trained to identify C auris cases. Every time a tertiary hospital has a Candida isolate similar to C auris or with some resistance, the LACEN and the Ministry of Health must be notified so that the reference center can confirm the identification,” he explained.
Almeida Júnior believes there are probably many people around the world who are on antibiotics and are hospitalized for a long time who end up in a state of hypercolonization and, subsequently, colonize the hospital environment. The way to confront the problem, he said, is to diagnose it quickly.
“We fear other hospitals may have patients with C auris without knowing it because there are no adequate diagnostic methods,” he said. This is why Anvisa is warning everyone.
The key message I would give Medscape readers is to “find out if your hospital’s laboratory is capable of identifying Candida auris,” he said.
The Role of the Pandemic
The first case of C auris in Brazil was reported during the pandemic, in December 2020. The fungus was isolated from the catheter tip sample of a patient without a history of hospitalization who had been admitted to a COVID-19 ICU at a hospital in Salvador. The patient required mechanical ventilation and hemodialysis. This case preceded an outbreak in 16 patients and led to two deaths.
Prohaska emphasized that using corticosteroids, which increases fungal proliferation, reusing personal protective equipment, and not changing gloves often enough are among the factors that could have contributed to the emergence of the fungus during the pandemic.
“For patients in serious condition, hospitalized for extended periods in ICUs or ward beds, the pandemic contributed to a series of opportunistic fungal infections,” Telles explained. A patient with severe COVID-19 who remains in the ICU for an extended period is exposed to a series of risk factors for candidemia, such as mechanical ventilation, catheters, antibiotics, and corticosteroids.
The main concern is invasive aspergillosis, followed by mucormycosis, or “black fungus disease,” and candidemia, he added. “If C auris colonizes something, the risk is very high.”
The first outbreak in Salvador showed that axillary monitoring thermometers were the main facilitator for the C auris outbreaks. “When I arrived at the hospital in Salvador, I went to the ICU, and my attention immediately turned to the axillary monitoring thermometers,” said Almeida Júnior, who credited a 2018 report published in the New England Journal of Medicine that alerted him to the idea that the thermometer could be the culprit.
At the time, the EpiSUS group was collecting data on the patients, so Almeida Júnior ordered cultures from thermometers. Eight of 47 (17%) were positive for C auris, the highest rate of positive cultures found on inanimate surfaces. On multivariate analysis, a colonized digital thermometer was the only independent risk factor associated with C auris colonization, his team reported.
“C auris highly colonizes patient axillae, and axillary monitoring thermometers are very difficult to sanitize,” said Almeida Júnior. “It is not enough to wipe them with alcohol. Ideally, they should be sanitized with hydrogen peroxide or replaced with an infrared thermometer.” This is what was done in Bahia. The hospital affected by the outbreak switched disinfectants, instituted new cleaning and disinfection practices and audits, and replaced the ICU’s axillary monitoring thermometers with infrared ones.
According to Almeida Júnior, more C auris outbreaks could be reported in Brazil, either in response to Anvisa’s warning or because of improvements in diagnostic methods, but he emphasized that the current focus is on the Northeast. He believes the Brazilian Northeastern coastline area might have a C auris niche, although this hypothesis has not been proven.
The fungus has also been found in beaches and saltwater bodies in India. “We have to identify whether the source is environmental,” said Almeida Júnior. “Together with national and international partners, we intend to study whether there is a C auris niche in the mangroves or beaches of the Brazilian Northeast.”
Prohaska, Almeida Júnior, and Telles stated there are no conflicts of interest.
Roxana Tabakman is a biologist, freelance reporter, and writer who resides in São Paulo, Brazil. She is the author of the books A saúde na Mídia, Medicina para Jornalistas, Jornalismo para Médicos (in Portuguese), and Biovigilados (in Spanish). Follow her on Twitter: @roxanatabakman.
This article originally appeared in the Portuguese edition of Medscape.
Follow Medscape on Facebook, Twitter, Instagram, and YouTube