Practice Essentials
True solitary thyroid nodules occur in 0.22-1.35% of the pediatric population and in close to 4% of the adult population. However, suspected thyroid nodules merit close attention in the pediatric population because such nodules are much more likely to be malignant in children than they are in adults. In addition, thyroid cancer is much more aggressive in children and is associated with early metastasis to regional lymph nodes and parenchymal organs, most commonly the lungs and bones. See the image below.
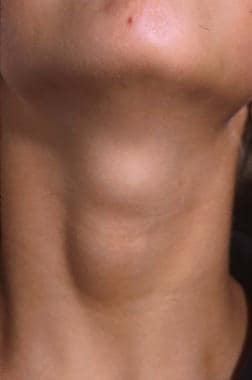
A 12-year-old patient with an asymptomatic palpable thyroid nodule noticed upon routine physical examination.
Signs and symptoms
Benign versus malignant nodules
Benign masses are usually movable, soft, and nontender. Malignancy is associated with a hard nodule, fixation to surrounding tissue, and regional lymphadenopathy.
Reported rapid growth or recurrent laryngeal nerve dysfunction found on examination may indicate malignancy and local infiltration.
If medullary carcinoma is suspected in conjunction with multiple endocrine neoplasia (MEN) 2B, multiple mucosal neuromas, marfanoid body habitus, and skeletal defects may be evident.
Hormonal imbalance
Although most patients are asymptomatic,
some exhibit signs and symptoms of altered levels of thyroid hormone, as follows:
Hyperthyroidism – Nervousness, heat intolerance, diarrhea, muscle weakness, and loss of weight and appetite; in rare cases, exophthalmos may be present in a person with a hyperfunctioning nodule
Hypothyroidism – May result in cold intolerance, constipation, fatigue, and weight gain, which, in children, is primarily caused by the accumulation of myxedematous fluid.
Nerve involvement
Signs and symptoms of local nerve involvement should trigger rapid investigation, because such involvement may be indicative of local invasiveness from malignancy. The most important of these signs are dysphagia and hoarseness.
See Clinical Presentation for more detail.
Diagnosis
Laboratory studies
Thyroid function tests – An elevated thyroid-stimulating hormone (TSH) level may indicate agenesis of a thyroid lobe or thyroiditis; a very low TSH level indicates an autonomous or hyperfunctioning nodule
Antithyroid antibodies – Helpful in diagnosing chronic lymphocytic thyroiditis (ie, Hashimoto thyroiditis)
Complete blood count (CBC) – If abscess is suspected
Calcium levels – Should be monitored immediately postoperatively to assess parathyroid function and the need for supplementation
Imaging studies
Ultrasonography – To determine whether the nodule is cystic, solid, or mixed
Radioiodine scintigraphy – To determine whether the nodule is cold, warm, or hot
Chest radiography – If malignancy is suspected, given the high incidence of early metastases to the lungs
Computed tomography (CT) scanning and magnetic resonance imaging (MRI) – To analyze the extent of disease by scanning the neck and chest
Histology
Follicular adenomas present the most common histology. These tumors maintain the follicular architecture of the gland and are usually encapsulated, without evidence of infiltration.
The 4 major malignancies that may be found in the thyroid gland are papillary carcinoma, follicular carcinoma, anaplastic carcinoma, and medullary thyroid cancer.
See Workup for more detail.
Management
Pharmacologic care and observation
Benign nodule – May simply be observed
Autoimmune thyroiditis – Treatment involves hormone replacement to maintain a euthyroid state
Infection – Abscesses should be drained and antibiotics administered
Warm nodule – A warm nodule without physical signs of malignancy is usually benign and may be observed with close follow-up for growth or change in the nodule
Hot nodule – A hot toxic nodule may require medical therapy before surgical removal; the patient should receive suppressive doses of antithyroid medications
Lobectomy
In the presence of a small, asymptomatic nodule, the surgeon may elect to perform a simple lobectomy with close follow-up observation. In such cases, full thyroid suppression also is recommended as lifetime postoperative therapy for the patient.
Nodule removal
All toxic nodules in children should be removed. In addition, if the presence of malignancy is still in question after diagnostic tests and procedures have been completed, perform surgical excision.
Total thyroidectomy
If any metastases are present, total thyroidectomy is the recommended treatment.
Thyroidectomy (near-total or total) may also be performed if Graves disease is diagnosed; thyroid hormone replacement therapy may not be needed if some tissue remains.
See Treatment and Medication for more detail.