Practice Essentials
Simple rib fractures are the most common injury sustained following blunt chest trauma, accounting for more than half of thoracic injuries from nonpenetrating trauma. Approximately 10% of all patients admitted after blunt chest trauma have one or more rib fractures.
These fractures are rarely life-threatening in themselves but can be an external marker of more severe visceral injury inside the abdomen and the chest.
First-rib fractures are considered indicators for increased morbidity and mortality in major trauma.
According to one study based on information in the UK Trauma Audit and Research Network, first-rib fracture was a significant predictor of injury severity (Injury Severity Score >15) and polytrauma.
In a study by Murphy et al, patients with a fracture of the first or second rib had higher mortality than patients with other rib fractures (7.4% vs 4.1%), as well as increased great vessel injury (2.8% vs 0.6%).
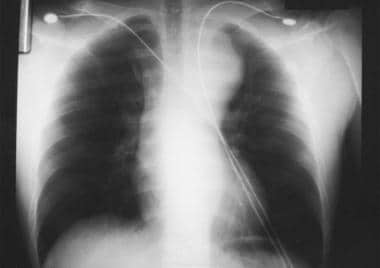
The image below depicts aortic injury, closely associated with a widening of greater than 8 cm measured at the widest points of the mediastinum.
Aortic injury is closely associated with a widening of greater than 8 cm measured at the widest points of the mediastinum on an upright anteroposterior chest radiograph.
The most common mechanism of injury for rib fractures in elderly persons is a fall from height or from standing. In adults, motor vehicle accident (MVA) is the most common mechanism. Youths sustain rib fractures most often secondary to recreational and athletic activities, as well as by nonaccidental trauma. Rib fractures may also be pathologic. Cancers that metastasize to bone (eg, prostate, breast, renal) frequently become apparent in a rib. Ribs are relatively thin compared with major long bones and are more likely to fracture when invaded by a metastatic lesion. In a study of Japanese patients with rheumatoid arthritis who were followed over a mean duration of 5.2 years, 13.5% reported incident fractures, with rib fractures being the most common fractures in men and vertebral fractures being the most common fractures in women, followed by rib fractures.
Anteroposterior (AP) and lateral chest films are used routinely to assist in the diagnosis of rib fractures, yet sensitivity as low as 50% has been reported. Delayed or follow-up radiographs can be very helpful. Obtaining a rib radiograph series remains controversial, as the additional information rarely changes the clinical picture or alters treatment. Rib detail radiographs can be helpful in evaluation of the 1st and 2nd ribs and the 7th through 12th ribs. Chest CT scan (see the image below) is more sensitive than plain radiographs for detecting rib fractures.
Because first and second rib fractures are often associated with vascular injury, ED physicians should consider angiography for such patients, especially if symptoms and signs of neurovascular compromise are present.
Pain control is fundamental to the management of rib fractures to decrease chest wall splinting and alveolar collapse in order to clear pulmonary secretions. Patients with minor rib injuries able to cough and clear secretions may be discharged with adequate analgesic medications. Intercostal nerve blocks provide pain relief without affecting respiratory function, although risks of this procedure include intravascular injection and pneumothorax. A small percentage of rib fractures do not heal even though a fibrous capsule may envelope the fracture. A nonunion may present months to years after injury and can cause discomfort with respiration due to movement of the fracture site.