Background
Epidural hematoma (EDH) is a traumatic accumulation of blood between the inner table of the skull and the stripped-off dural membrane. EDH results from traumatic head injury, usually with an associated skull fracture and arterial laceration.The inciting event often is a focused blow to the head, such as that produced by a hammer or baseball bat. In 85-95% of patients, this type of trauma results in an overlying fracture of the skull. Blood vessels in close proximity to the fracture are the sources of the hemorrhage in the formation of an epidural hematoma. Because the underlying brain has usually been minimally injured, prognosis is excellent if treated aggressively. Outcome from surgical decompression and repair is related directly to patient’s preoperative neurologic condition.
In a study of 41 patients with epidural hematoma at a level I trauma center, the patients’ age, severity of traumatic brain injury, and neurologic status were the main factors influencing outcome. Two patients died within 24hours, and 39 patients (95%) survived. Thirty-two patients (78%) showed good recovery at latest follow-up.
In cases of rare bilateral extradural hematoma (0.5-10%), higher mortality has been reported. Approach to treatment depends on the volume, time of diagnosis, and neurologic deficit level. Simultaneous drainage of bilateral hematomas has been demonstrated to be an effective technique.
See the images below.
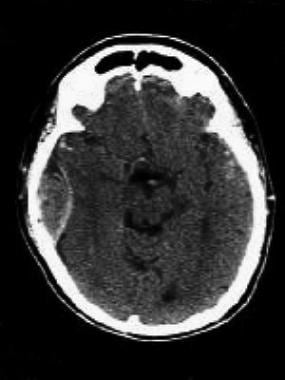
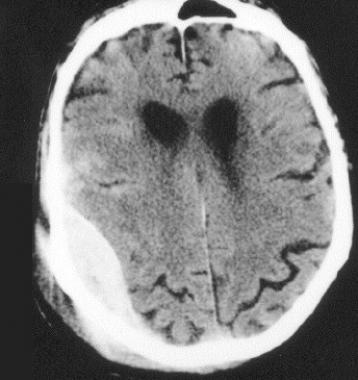
Right temporal epidural hematoma with midline shift. Patient should be taken immediately to the operating room for neurosurgery. This may require emergent transport to a trauma center or other facility with a neurosurgeon available.
Brain CT scan of 90-year-old man who slipped on a waxed floor. Witnesses reported loss of consciousness followed by a “lucid interval.” Patient arrived to ED unconscious. CT scan indicates epidural hematoma. Image courtesy of Dr Dana Stearns, Massachusetts General Hospital.