Practice Essentials
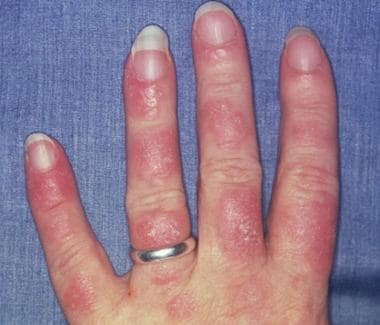
Systemic lupus erythematosus (SLE) is an autoimmune disorder characterized by antibodies to nuclear and cytoplasmic antigens, multisystem inflammation, protean clinical manifestations, and a relapsing and remitting course. More than 90% of cases of SLE occur in women, frequently starting at childbearing age. See the image below.
Photosensitive systemic lupus erythematosus (SLE) rashes typically occur on the face or extremities, which are sun-exposed regions. Although the interphalangeal spaces are affected, the metacarpophalangeal (MCP) and proximal interphalangeal (PIP) and distal interphalangeal (DIP) joints are spared. Photo courtesy of Dr. Erik Stratman, Marshfield Clinic.
See Cutaneous Clues to Accurately Diagnosing Rheumatologic Disease, a Critical Images slideshow, to help recognize cutaneous manifestations of rheumatologic diseases. Also, see the Autoimmune Disorders: Making Sense of Nonspecific Symptoms slideshow to help identify several diseases that can cause a variety of nonspecific symptoms.
Signs and symptoms of SLE
SLE is a chronic inflammatory disease that can affect almost any organ system, although it mainly involves the skin, joints, kidneys, blood cells, and nervous system. Its presentation and course are highly variable, ranging from indolent to fulminant.
In childhood-onset SLE, the following clinical manifestations are more commonly found than in adults
:
Malar rash
Ulcers/mucocutaneous involvement
Kidney involvement, proteinuria, urinary cellular casts
Seizures
Thrombocytopenia
Hemolytic anemia
Fever
Lymphadenopathy.
In adults, Raynaud pleuritis and sicca are twice as common as in children and adolescents.
The classic presentation of a triad of fever, joint pain, and rash in a woman of childbearing age should prompt investigation into the diagnosis of SLE.
Patients may present with any of the following manifestations
:
Constitutional (eg, fatigue, fever, arthralgia, weight changes)
Musculoskeletal (eg, arthralgia, arthropathy, myalgia, frank arthritis, avascular necrosis)
Dermatologic (eg, malar rash, photosensitivity, discoid lupus)
Renal (eg, acute or chronic kidney failure, acute nephritic disease)
Neuropsychiatric (eg, seizure, psychosis)
Pulmonary (eg, pleurisy, pleural effusion, pneumonitis, pulmonary hypertension, interstitial lung disease)
Gastrointestinal (eg, nausea, dyspepsia, abdominal pain)
Cardiac (eg, pericarditis, myocarditis)
Hematologic (eg, cytopenias such as leukopenia, lymphopenia, anemia, or thrombocytopenia)
In patients with suggestive clinical findings, a family history of autoimmune disease should raise further suspicion of SLE.
See Presentation for more detail.
Diagnosis of SLE
The diagnosis of SLE is based on a combination of clinical findings and laboratory evidence. Familiarity with the diagnostic criteria helps clinicians to recognize SLE and to subclassify this complex disease based on the pattern of target-organ manifestations.
The American College of Rheumatology (ACR) and the European League Against Rheumatism (EULAR) published new criteria for the classification of SLE in 2019.
These criteria represent current concepts of SLE, and have excellent specificity and sensitivity. They replace the 1997 ACR criteria for SLE diagnosis.
The ACR/EULAR classification requires an antinuclear antibody (ANA) titer of at least 1:80 on HEp-2 cells or an equivalent positive test at least once. If that is present, 22 “additive weighted” classification criteria are considered, comprising seven clinical domains (constitutional, hematologic, neuropsychiatric, mucocutaneous, serosal, musculoskeletal, renal) and three immunologic domains (antiphospholipid antibodies, complement proteins, SLE-specific antibodies).
Each criterion is assigned points, ranging from 2 to 10. Patients with at least one clinical criterion and 10 or more points are classified as having SLE. See Workup.
Testing
Laboratory studies used in the diagnosis of SLE are as follows:
CBC with differential
Serum creatinine
Urinalysis with microscopy
ESR or CRP level
Complement levels
Liver function tests
Creatine kinase assay
Spot protein/spot creatinine ratio
Autoantibody tests
Imaging studies
The following imaging studies may be used to evaluate patients with suspected SLE:
Joint radiography
Chest radiography and chest CT scanning
Echocardiography
Brain MRI/MRA
Cardiac MRI
Procedures
Procedures that may be performed in patients with suspected SLE include the following:
Arthrocentesis
Lumbar puncture
Kidney biopsy
See Workup for more detail.
Management
Management of SLE often depends on the individual patient’s disease severity and disease manifestations,
although hydroxychloroquine has a central role for long-term treatment in all SLE patients.
Pharmacotherapy
Medications used to treat SLE manifestations include the following:
Antimalarials (eg, hydroxychloroquine)
Corticosteroids (eg, methylprednisolone, prednisone), short-term use recommended
Nonbiologic DMARDS: Cyclophosphamide, methotrexate, azathioprine, mycophenolate, cyclosporine
Nonsteroidal anti-inflammatory drugs (NSAIDS; eg, ibuprofen, naproxen, diclofenac)
Biologic DMARDs (disease-modifying antirheumatic drugs): Belimumab, rituximab, anifrolumab, and/or IV immune globulin
See Treatment and Medication for more detail.
See also the following Medscape articles:
Pediatric Systemic Lupus Erythematosus