Practice Essentials
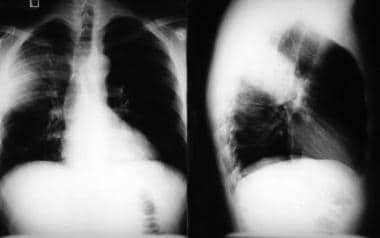
Bacterial pneumonia (see the image below) is caused by a pathogenic infection of the lungs and may present as a primary disease process or as the final, fatal disorder primarily in an individual who is already debilitated. The most consistent presenting symptom of bacterial pneumonia is cough productive of sputum. Antibiotic treatment is the mainstay of drug therapy for bacterial pneumonia.
Bacterial pneumonia. Radiographic images in a patient with right upper lobe pneumonia. Note the increased anteroposterior chest diameter, which is suggestive of chronic obstructive pulmonary disease (COPD).
Signs and symptoms of bacterial pneumonia
Cough, particularly cough productive of sputum, is the most consistent presenting symptom of bacterial pneumonia and may suggest a particular pathogen, as follows:
Streptococcus pneumoniae: Rust-colored sputum
Pseudomonas, Haemophilus, and pneumococcal species: May produce green sputum
Klebsiella species pneumonia: Red currant-jelly sputum
Anaerobic infections: Often produce foul-smelling or bad-tasting sputum
Signs of bacterial pneumonia may include the following:
Hyperthermia (fever, typically >38°C)
or hypothermia (< 35°C)
Tachypnea (>18 respirations/min)
Use of accessory respiratory muscles
Tachycardia (>100 bpm) or bradycardia (< 60 bpm)
Central cyanosis
Altered mental status
Physical findings may include the following:
Adventitious breath sounds, such as rales/crackles, rhonchi, or wheezes
Decreased intensity of breath sounds
Egophony
Whispering pectoriloquy
Dullness to percussion
Tracheal deviation
Lymphadenopathy
Pleural friction rub
Examination findings that may indicate a specific etiology include the following:
Bradycardia: May indicate a Legionella etiology
Periodontal disease: May suggest an anaerobic and/or polymicrobial infection
Cutaneous nodules: May suggest Nocardia infection
Decreased gag reflex: Suggests risk for aspiration
See Clinical Presentation for more detail.
Diagnosis of bacterial pneumonia
Severity assessment
Tools to assess the severity of disease and risk of death include the PSI/PORT (ie, pneumonia severity index/Patient Outcomes Research Team score), the CURB-65 (ie, confusion, urea, respiratory rate, blood pressure, and age >65 years) system, and the APACHE (ie, acute physiology and chronic health evaluation), among others.
The following laboratory tests are also useful for assessing illness severity:
Serum chemistry panel
Arterial blood gas (ABG) determination
Venous blood gas determination (central venous oxygen saturation)
Complete blood cell (CBC) count with differential
Serum free cortisol value
Serum lactate level
Sputum evaluation
Sputum Gram stain and culture should be performed before initiating antibiotic therapy. A single predominant microbe should be noted at Gram staining, although mixed flora may be observed with anaerobic infection caused by aspiration.
Imaging studies
Chest radiography: The criterion standard for establishing the diagnosis of pneumonia
Chest computed tomography scanning
Chest ultrasonography
Bronchoscopy
Lung tissue can be visually evaluated and bronchial washing specimens can be obtained with the aid of a fiberoptic bronchoscope. Protected brushings and bronchoalveolar lavage (BAL) can be performed for fluid analysis and cultures.
Thoracentesis
This is an essential procedure in patients with a parapneumonic pleural effusion. Analysis of the fluid allows differentiation between simple and complicated effusions.
Pathogen-specific tests
Urine assays
Sputum, serum, and/or urinary antigen tests
Immune serologic tests
Histologic examination
Histologic inflammatory lung changes vary according to whether the patient has lobar pneumonia, bronchopneumonia, or interstitial pneumonia.
See Workup for more detail.
Management of bacterial pneumonia
The mainstay of drug therapy for bacterial pneumonia is antibiotic treatment. First-line antimicrobials for S pneumoniae, the most prevalent cause of bacterial pneumonia, are, for the penicillin-susceptible form of the bacterium, penicillin G and amoxicillin. For the penicillin-resistant form of S pneumoniae, first-line agents are chosen on the basis of sensitivity.
Supportive measures include the following:
Analgesia and antipyretics
Chest physiotherapy
Intravenous fluids (and, conversely, diuretics), if indicated
Pulse oximetry with or without cardiac monitoring, as indicated
Oxygen supplementation
Positioning of the patient to minimize aspiration risk
Respiratory therapy, including treatment with bronchodilators and N-acetylcysteine
Suctioning and bronchial hygiene
Ventilation with low tidal volumes (6 mL/kg of ideal body weight) in patients requiring mechanical ventilation secondary to bilateral pneumonia or acute respiratory distress syndrome (ARDS)
Systemic support: May include proper hydration, nutrition, and mobilization
See Treatment and Medication for more detail.