Practice Essentials
In approximately 1/3 of patients with epilepsy, seizures persist despite adequate trials of several antiepileptic drugs (AEDs). Surgery can provide seizure freedom for some patients with seizures resistant to AEDs.
Criteria for surgical intervention
A candidate for epilepsy surgery must have not attained acceptable seizure control with sufficient trials of AEDs and must have a reasonable chance of benefiting from surgery. The American Academy of Neurology, the American Association of Neurological Surgeons, and the American Epilepsy Society have recommended the following practice parameters
:
Patients with disabling complex partial seizures, with or without secondarily generalized seizures, who have failed appropriate trials of first-line AEDs, should be considered for referral to an epilepsy surgery center, though criteria for failure of drug treatment have not been definitely established (level A)
Patients referred to an epilepsy center for the reasons stated above who meet established criteria for anteromedial temporal resection (AMTR) and who will accept the risks and benefits of this procedure, as opposed to continuing pharmacotherapy, should be offered surgical treatment (level A)
Preoperative assessment and surgical strategy
Modalities used for evaluation of seizures include the following:
Neuroimaging – Skull radiography, CT, MRI, positron emission tomography (PET), single-photon emission CT (SPECT), and magnetoencephalography/magnetic source imaging (MEG/MSI)
Electroencephalography (EEG; the single most useful test in epilepsy diagnosis)
Neuropsychological (neurocognitive) testing
Intracarotid amobarbital (Wada) test
Invasive intracranial monitoring (eg, intracranial EEG recording, or chronic electrocorticography [ECoG])
The surgical strategy may be either definitive or palliative, as follows:
Definitive – The aim is to produce complete, or at least 70-90%, improvement in seizures; in general, these procedures physically remove seizure-producing cortex from the brain
Palliative – The aim is to decrease seizure frequency (seizure freedom is rare); these procedures usually disrupt pathways involved in seizure production and propagation or attempt to disrupt seizures with the use of electrical stimulation
Surgical techniques
The following 4 procedures may be considered for the surgical treatment of epilepsy:
Anteromedial temporal resection (AMTR) – This is the most commonly performed procedure, with the clearest indications and best results
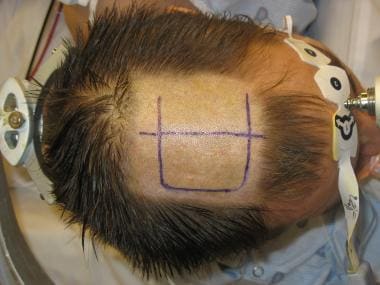
Corpus callosotomy – The aim of this procedure is to disrupt 1 or more major central nervous system (CNS) pathways used in seizure generalization, thus reducing the frequency and severity of primary or secondary generalized seizures (see the image below)
Surgical site preparation for corpus callosotomy. Right hemisphere is inferior, and left hemisphere is superior. In this position, left hemisphere will be held out of field by falx cerebri, and right hemisphere will fall away from field, minimizing need for traction.
Multiple subpial transection (MST) – The aim of this nonresective procedure is to abolish epileptiform discharges and correlative seizures from epileptogenic cortex by disrupting intracortical synchronization and thereby (theoretically) reducing or eliminating the epileptogenic potential of the seizure focus
Functional hemispherectomy – In this procedure, the cortex is disconnected from all subcortical structures, and the interhemispheric commissures are divided, but the brain remains in place
Postoperative complications that may occur include the following:
AMTR – Hemiparesis, visual field deficit, infections, cranial nerve palsy, fever, verbal deficits and memory problems
Corpus callosotomy – Hydrocephalus, aseptic meningitis, bleeding from the superior sagittal sinus, frontal lobe edema, venous infarction, and air embolism
Functional hemispherectomy – Hemogenic meningitis, ventriculitis, cerebrospinal fluid leakage, and hydrocephalus; less commonly, stroke, infection, coma, and postoperative hemorrhage