Practice Essentials
Psoriatic arthritis is most commonly a seronegative oligoarthritis found in patients with psoriasis, with less common, but characteristic, differentiating features of distal joint involvement and arthritis mutilans.
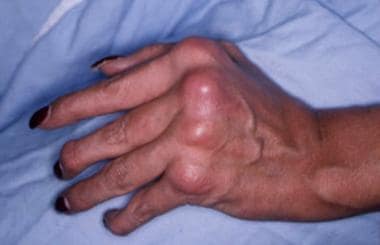
One in five patients with psoriasis has psoriatic arthritis (see the image below).
Swelling and deformity of the metacarpophalangeal and distal interphalangeal joints in a patient with psoriatic arthritis.
See Psoriasis: Manifestations, Management Options, and Mimics, a Critical Images slideshow, to help recognize the major psoriasis subtypes and distinguish them from other skin lesions. Go to Psoriatic Arthritis Decision Point for expert commentary on psoriatic arthritis diagnosis and treatment decisions and related guidelines.
Signs and symptoms
Onset of psoriasis and arthritis are as follows:
Psoriasis appears to precede the onset of psoriatic arthritis in 60-80% of patients (occasionally by as many as 20 years, but usually by less than 10 years)
In as many as 15-20% of patients, arthritis appears before the psoriasis
Occasionally, arthritis and psoriasis appear simultaneously
In some cases, patients may experience only stiffness and pain, with few objective findings. In most patients, the musculoskeletal symptoms are insidious in onset, but an acute onset has been reported in one third of all patients.
Findings on physical examination are as follows:
Enthesopathy or enthesitis, reflecting inflammation at tendon or ligament insertions into bone, is observed more often at the attachment of the Achilles tendon and the plantar fascia to the calcaneus with the development of insertional spurs
Dactylitis with sausage digits is seen in as many as 35% of patients
Skin lesions include scaly, erythematous plaques; guttate lesions; lakes of pus; and erythroderma
Psoriasis may occur in hidden sites, such as the scalp (where psoriasis frequently is mistaken for dandruff), perineum, intergluteal cleft, and umbilicus
Psoriatic nail changes, which may be a solitary finding in patients with psoriatic arthritis, may include the following:
Beau lines
Leukonychia
Onycholysis
Oil spots
Subungual hyperkeratosis
Splinter hemorrhages
Spotted lunulae
Transverse ridging
Cracking of the free edge of the nail
Uniform nail pitting
Extra-articular features are observed less frequently in patients with psoriatic arthritis than in those with rheumatoid arthritis (RA) but may include the following:
Synovitis affecting flexor tendon sheaths, with sparing of the extensor tendon sheath
Subcutaneous nodules are rare
Ocular involvement may occur in 30% of patients, including conjunctivitis in 20% and acute anterior
uveitis in 7%; in patients with uveitis, 43% have
sacroiliitis
Patterns of arthritic involvement
The patterns of psoriatic arthritis involvement are as follows:
Asymmetrical oligoarticular arthritis
Symmetrical polyarthritis
Distal interphalangeal arthropathy
Arthritis mutilans
Spondylitis with or without sacroiliitis
See Presentation for more detail.
Diagnosis
Classification of psoriatic arthritis
The Classification Criteria for Psoriatic Arthritis (CASPAR)
consist of established inflammatory articular disease with at least 3 points from the following features:
Current psoriasis (assigned a score of 2)
A history of psoriasis (in the absence of current psoriasis; assigned a score of 1)
A family history of psoriasis (in the absence of current psoriasis and history of psoriasis; assigned a score of 1)
Dactylitis (assigned a score of 1)
Juxta-articular new-bone formation (assigned a score of 1)
RF negativity (assigned a score of 1)
Nail dystrophy (assigned a score of 1)
Laboratory findings
No specific diagnostic tests are available for psoriatic arthritis.
The most characteristic laboratory abnormalities in patients with the condition are as follows:
Elevations of the erythrocyte sedimentation rate (ESR) and C-reactive protein level
Negative rheumatoid factor in 91-95% of patients
In 10-20% of patients with generalized skin disease, the serum uric acid concentration may be increased
Low levels of circulating immune complexes have been detected in 56% of patients
Serum immunoglobulin A levels are increased in two thirds of patients
Synovial fluid is inflammatory, with cell counts ranging from 5000-15,000/µL and with more than 50% of cells being polymorphonuclear leukocytes; complement levels are either within reference ranges or increased, and glucose levels are within reference ranges
Radiographic studies
Radiologic features have helped to distinguish psoriatic arthritis from other causes of polyarthritis. In general, the common subtypes of psoriatic arthritis, such as asymmetrical oligoarthritis and symmetrical polyarthritis, tend to result in only mild erosive disease. Early bony erosions occur at the cartilaginous edge, and cartilage is initially preserved, with maintenance of a normal joint space.
The following radiographic abnormalities are suggestive of psoriatic arthritis:
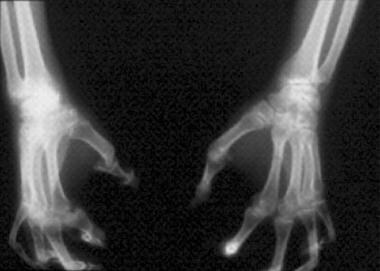
Pencil-in-cup deformity (erosion of the distal end of the phalanx into a sharpened pencil shape, with the proximal surface of the adjoining phalanx worn into a cup shape; see the image below)
Arthritis mutilans (ie, “pencil-in-cup” deformities).
Joint-space narrowing in the interphalangeal joints, possibly with ankylosis
Increased joint space in the interphalangeal joints as a result of destruction
Fluffy periostitis
Bilateral, asymmetrical, fusiform soft-tissue swelling
Unilateral or symmetrical sacroiliitis
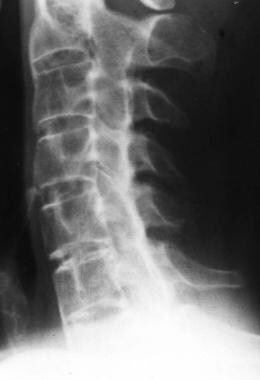
Large, nonmarginal, unilateral, asymmetrical syndesmophytes (intervertebral bony bridges, seen in the image below) in the cervical, thoracic, and lumbar spine, often sparing some of the segments
Lateral radiograph of the cervical spine shows syndesmophytes at the C2-3 and C6-7 levels, with zygapophyseal joint fusion. Courtesy of Bruce M. Rothschild, MD.
Magnetic resonance imaging studies
Particularly sensitive for detecting sacroiliitic synovitis, enthesitis, and erosions; can also be used with gadolinium to increase sensitivity
May show inflammation in the small joints of the hands, involving the collateral ligaments and soft tissues around the joint capsule, a finding not seen in persons with RA
See Workup for more detail.
Management
Medical treatment regimens include the use of nonsteroidal anti-inflammatory drugs (NSAIDs), Janus kinase (JAK) inhibitors, and disease-modifying antirheumatic drugs (DMARDs). DMARDs include the following
:
Methotrexate
Sulfasalazine
Cyclosporine
Leflunomide
Biologic agents (eg, TNF, PDE4, or interleukin inhibitors; CD80 binders)
In patients with severe skin inflammation, medications such as methotrexate, retinoic-acid derivatives, and psoralen plus ultraviolet (UV) light should be considered. These agents have been shown to work on skin and joint manifestations. Intra-articular injection of entheses or single inflamed joints with corticosteroids may be particularly effective in some patients. Use DMARDs in individuals whose arthritis is persistent.
Surgical care
Arthroscopic synovectomy has been effective in treating severe, chronic, monoarticular synovitis
Joint replacement and forms of reconstructive therapy are occasionally necessary
Patients in severe pain or with significant contractures may be referred for possible surgical intervention; however, high rates of recurrence of joint contractures have been noted after surgical release, especially in the hand
Hip and knee joint replacements have been successful
Arthrodesis and arthroplasty have also been used on joints, such as the proximal interphalangeal joint of the thumb
The wrist often spontaneously fuses, and this may relieve the patient’s pain without surgical intervention
For arthritis mutilans, surgical intervention is usually directed toward salvage of the hand; combinations of arthrodesis, arthroplasty, and bone grafts to lengthen the digits may be used
Physical therapy
The rehabilitation treatment program for patients with psoriatic arthritis should be individualized and should be started early in the disease process. Such a program should consider the use of the following:
Rest: Local and systemic
Exercise: Passive, active, stretching, strengthening, and endurance
Modalities: Heat, cold
Orthotics: Upper and lower extremities, spinal
Assistive devices for gait and adaptive devices for self-care tasks: Including possible modifications to homes and automobiles
Education about the disease, energy conservation techniques, and joint protection
Possible vocational readjustments
See Treatment and Medication for more detail.