Practice Essentials
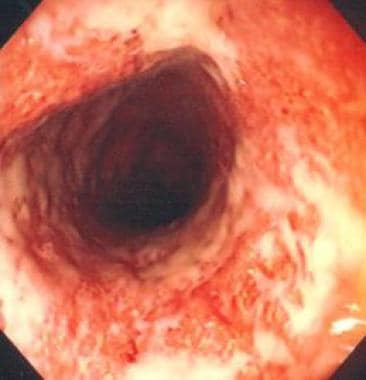
Ulcerative colitis (UC) is one of the two major types of inflammatory bowel disease (IBD), along with Crohn disease (CD). Unlike Crohn disease, which can affect any part of the gastrointestinal tract, ulcerative colitis characteristically involves the large bowel (see the image below). Ulcerative colitis is a lifelong illness that has a profound emotional and social impact on the affected patients.
Ulcerative colitis. Ulcerative colitis as visualized with a colonoscope.
Signs and symptoms
Patients with UC predominantly complain of the following:
Rectal bleeding
Frequent stools
Mucous discharge from the rectum
Tenesmus (occasionally)
Lower abdominal pain and severe dehydration from purulent rectal discharge (in severe cases, especially in the elderly)
In some cases, UC has a fulminant course marked by the following:
Severe diarrhea and cramps
Fever
Leukocytosis
Abdominal distention
UC is associated with various extracolonic manifestations, as follows:
Uveitis
Pyoderma gangrenosum
Pleuritis
Erythema nodosum
Ankylosing spondylitis
Spondyloarthropathies
Other conditions associated with UC include the following:
Primary sclerosing cholangitis (PSC)
Recurrent subcutaneous abscesses unrelated to pyoderma gangrenosum
Multiple sclerosis
Immunobullous disease of the skin
Physical findings are typically normal in mild disease, except for mild tenderness in the lower left abdominal quadrant (tenderness or cramps are generally present in moderate to severe disease
). In severe disease, the following may be observed:
Fever
Tachycardia
Significant abdominal tenderness
Weight loss
The severity of UC can be graded as follows:
Mild: Bleeding per rectum, fewer than four bowel motions per day
Moderate: Bleeding per rectum, more than four bowel motions per day
Severe: Bleeding per rectum, more than four bowel motions per day, and a systemic illness with hypoalbuminemia (< 30 g/L)
See Presentation for more detail.
Diagnosis
Laboratory studies are useful principally in determining the extent of the disease, excluding other diagnoses, and in assessing the patient’s nutritional status. They may include the following:
Serologic markers (eg, antineutrophil cytoplasmic antibodies [ANCA], anti– Saccharomyces cerevisiae antibodies [ASCA])
Complete blood cell (CBC) count
Comprehensive metabolic panel
Inflammation markers (eg, erythrocyte sedimentation rate [ESR], C-reactive protein [CRP])
Stool assays
Diagnosis is best made with endoscopy and biopsy, on which the following are characteristic findings:
Abnormal erythematous mucosa, with or without ulceration, extending from the rectum to a part or all of the colon
Uniform inflammation, without intervening areas of normal mucosa (skip lesions tend to characterize Crohn disease)
Contact bleeding may also be observed, with mucus identified in the lumen of the bowel
The extent of disease is defined by the following findings on endoscopy:
Extensive disease: Evidence of UC proximal to the splenic flexure
Left-side disease: UC present in the descending colon up to, but not proximal to, the splenic flexure
Proctosigmoiditis: Disease limited to the rectum with or without sigmoid involvement
Imaging modalities that may be considered include the following:
Plain abdominal radiography
Double-contrast barium enema examination
Cross-sectional imaging studies (eg, ultrasonography, magnetic resonance imaging, computed tomography scanning)
Radionuclide studies
Angiography
See Workup for more detail.
Management
Medical treatment of mild UC includes the following:
Mild disease confined to the rectum: Topical mesalazine via suppository (preferred) or budesonide rectal foam
Left-side colonic disease: Mesalazine suppository and oral aminosalicylate (oral mesalazine is preferred to oral sulfasalazine)
Systemic steroids, when disease does not quickly respond to aminosalicylates
Oral budesonide
After remission, long-term maintenance therapy (eg, once-daily mesalazine)
Medical treatment of acute, severe UC may include the following:
Hospitalization
Intravenous high-dose corticosteroids
Alternative induction medications: Cyclosporine, tacrolimus, infliximab, adalimumab, golimumab
Indications for urgent surgery include the following:
Toxic megacolon refractory to medical management
Fulminant attack refractory to medical management
Uncontrolled colonic bleeding
Indications for elective surgery include the following:
Long-term steroid dependence
Dysplasia or adenocarcinoma found on screening biopsy
Disease being present for 7-10 years
Surgical options include the following
:
Total colectomy (panproctocolectomy) and ileostomy
Total colectomy
Ileoanal pouch reconstruction or ileorectal anastomosis
In an emergency, subtotal colectomy with end-ileostomy
See Treatment and Medication for more detail.