Background
Although pacemakers provide relief from life-threatening arrhythmias and can improve quality of life significantly, they also can function in a nonphysiologic manner, which is accompanied by nontrivial morbidity. Ventricular pacing has been noted to sacrifice the atrial contribution to ventricular output; in some instances, atrial contraction occurs against closed atrioventricular (AV) valves, producing reverse blood flow and nonphysiologic pressure waves.
McWilliam described a reduction in blood pressure in response to electrical stimulation of a cat’s ventricle in 1889.
Since the first pacemaker was implanted in 1958, investigators have reported decreased cardiac output in humans as a response to ventricular pacing (see the Cardiac Output calculator). In response to decreased cardiac output, the majority of patients demonstrate aortic and carotid baroreceptor reflex activity, which increases total peripheral resistance (TPR) to maintain constant blood pressure. In some patients, TPR does not increase in response to decreased cardiac output, which results in decreased blood pressure.
The combination of decreased cardiac output, loss of atrial contribution to ventricular filling, loss of TPR response, and nonphysiologic pressure waves contributes to symptoms collectively known as pacemaker syndrome.
The definition of pacemaker syndrome has evolved and been the subject of discussion since 1969, when Mitsui and colleagues first reported a constellation of symptoms they thought to be rate-related in patients with ventricular pacemakers.
Successive definitions have sought to include data from later investigations into the pathophysiology of the symptoms produced. Furman redefined pacemaker syndrome in a 1994 editorial in which he included the following elements
:
Loss of AV synchrony
Retrograde ventriculoatrial (VA) conduction
Absence of rate response to physiologic need
Ellenbogen and colleagues focused on clinical utility and proposed that “pacemaker syndrome represents the clinical consequences of AV dyssynchrony or suboptimal AV synchrony, regardless of the pacing mode.”
Recently, most authors have recognized that pacemaker syndrome, which initially was described in patients with ventricular pacemakers, is related to nonphysiologic timing of atrial and ventricular contractions, which may occur in a variety of pacing modes. Some have proposed renaming the syndrome “AV dyssynchrony syndrome,” which more specifically reflects the mechanism responsible for symptom production.
AV dyssynchrony may occur outside the setting of pacemakers, however, as noted by Furman, who described the following nonpacing conditions
:
Extremely prolonged first-degree AV block
Nodal rhythm more rapid than the atrial rate, as might occur in children with sinus node dysfunction after congenital defect repair
Such examples have been termed “pseudo pacemaker syndrome,” in an effort to reserve the term pacemaker syndrome only for cases involving pacemakers. Other examples of pseudo pacemaker syndrome have been described, including hypertrophic cardiomyopathy with complete AV block.
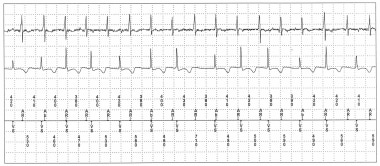
Pseudo pacemaker syndrome may occur in the setting of an implanted pacemaker when the pacemaker does not participate significantly in creation of AV dyssynchrony. One example is demonstrated in the figure below, which is an example of atrial tachycardia with Wenckebach-type, second degree AV block that results in significant AV dyssynchrony. The patient exhibited symptoms of pacemaker syndrome, including fatigue, lightheadedness, and exertional dyspnea.
Pacemaker syndrome without pacemaker participation. Displayed are stored data from a dual-chamber pacemaker. The intracardiac tracings reveal atrial tachycardia with second-degree AV block that together created continuous atrioventricular (AV) dyssynchrony, leading to symptoms of pacemaker syndrome, including fatigue, lightheadedness, and exertional dyspnea. Notice that the pacemaker does not participate in creation of AV dyssynchrony. There are no paced events. Top tracing: atrial electrogram. Middle tracing: ventricular electrogram. Bottom tracing: channel markers. Ab = atrial sensed event in postventricular blanking period, AR = atrial sensed event in postventricular refractory period; VS – Ventricular sensed event.
The working definition of pacemaker syndrome currently includes the following:
A constellation of specific symptoms occurs.
Symptoms occur in the setting of a pacemaker, temporary or permanent.
Symptoms result from loss of physiologic timing of atrial and ventricular contractions.
The last condition may be unnecessary, and it helps blur the distinction between definition of syndrome and elucidation of cause. It also excludes at least one mechanism known to contribute to production of the constellation of symptoms, specifically, ventricular activation pattern.