Practice Essentials
Status epilepticus (SE) is a common, life-threatening neurologic disorder that is essentially an acute, prolonged epileptic crisis (see the image below). SE can represent an exacerbation of a preexisting seizure disorder or the initial manifestation of a seizure disorder (epilepsy), or it can represent an insult other than a seizure disorder. Among such insults, SE can occur in the context of an acute cerebral injury, or be due to a systemic process or illness, in a patient with or without a remote cerebral injury. In patients with known epilepsy, the most common cause of SE is a change in medication. Most seizures terminate spontaneously; SE represents a failure of seizure termination.
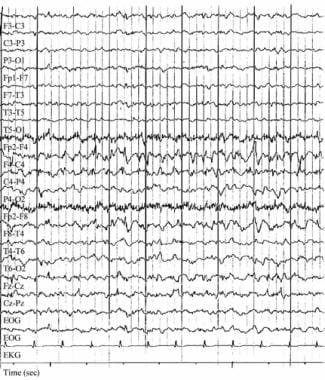
Focal status epilepticus. Electroencephalograph (EEG) in a patient with epilepsia partialis continua caused by Rasmussen encephalitis before hemispherectomy. The patient had long-standing, intractable partial epilepsy since the first decade of life. Seizures included complex partial with occasional secondary generalization and repetitive myoclonus involving the left side of the body. Note the frequent epileptiform discharges at 1-2 Hz involving the right frontocentral channels. These were evident on many of the patient’s routine EEGs. Clinical myoclonus is often correlated with high-voltage bursts of such activity.
Signs and symptoms
By clinical history, nonmotor simple partial status epilepticus involves subjective sensory disturbances, including the following:
Focal or unilateral paresthesias or numbness
Focal visual changes, usually characterized by flashing lights
Focal visual obscuration or focal colorful hallucinations
Olfactory or gustatory hallucinations
Atypical rising abdominal sensations
Epilepsy partialis continua, or focal status epilepticus of the motor cortex, may occur in various contexts, with some authors subdividing it into type I (nonprogressive) and type II (progressive).
Type I epilepsy partialis continua features include the following:
Intermittent, semi-rhythmic, involuntary twitching involving a discrete subset of muscles
Most commonly affects the face and ipsilateral distal hand musculature
Myoclonus of this variety may evolve into partial or generalized convulsion
Type II epilepsy partialis continua features include the following:
Usually linked with Rasmussen encephalitis
Gradual loss of unilateral function, with parallel focal or unilateral hemispheric atrophy
Impaired intellectual skills to various degrees
Possible effect on language skills
Type I complex partial status epilepticus refers to recurrent, recognizable complex partial seizures without recovery between seizures. Type II represents continuous, ongoing complex partial seizure activity. The sequence of constellation of features in complex partial status epilepticus is as follows:
Serious medical, surgical, or neurologic illness
A brief convulsive seizure
Protracted stupor with fluctuating neurologic findings, subtle nystagmus, or focal twitching
In addition, complex partial status epilepticus may have the following characteristics:
History of recurrent or prolonged simple partial seizures or may follow or precede a generalized convulsive seizure
Confused and variable responsiveness; fluctuating or bizarre behavior
Impaired memory of the event
Clinical automatisms (eg, repetitive lip-smacking, fumbling, swallowing movements)
Subtle nystagmus
See Clinical Presentation for more detail.
Diagnosis
Examination for status epilepticus includes the following:
Generalized convulsive status epilepticus: Typical rhythmic tonic-clonic activity, impaired consciousness; rarely, may present as persistent tonic seizure
Status epilepticus due to the use of illicit, or street, drugs: needle-track marks
Status epilepticus due to possible mass lesion or brain infection: Papilledema, lateralized neurologic features
Subtle or transformed status epilepticus: Any patient without improving level of consciousness within 20–30 minutes of cessation of generalized seizure activity; ocular and fine motor findings such as nystagmus, pupillary hippus, or myoclonic or clonic movements of a hand, foot, digit or face.
Associated injuries in patients with seizures: May include tongue lacerations (typically lateral), shoulder dislocations, head trauma, facial trauma
Classification
The Luders and Rona semiologic classification consists of 3 axes, as follows
:
The type of brain function predominantly compromised
The body part involved
The evolution over time
The Treiman classification is as follows:
Generalized convulsive status epilepticus
Subtle status epilepticus
Nonconvulsive status epilepticus (eg, absence, complex partial)
Simple partial status epilepticus
The International League Against Epilepsy (ILAE) classification
consists of 4 axes, as follows:
Semiology – including those with or without prominent motor findings
Etiology – known and unknown causes
EEG correlates – description of the EEG
Age – neonatal, infancy, childhood, adolescent, adult, and elderly
Testing
The workup for potential status epilepticus is similar to that for any self-limited seizure but is done more expeditiously to confirm the diagnosis and to abort or limit the seizures.
Stat laboratory studies that should be obtained include the following:
Glucose and electrolyte levels (including calcium, magnesium)
Complete blood count
Renal and liver function tests
Toxicologic screening and anticonvulsant drug levels
Arterial blood gas results
Other tests that may be appropriate depending on the clinical setting include the following:
Electroencephalography: Criterion standard for diagnosing status epilepticus
; however, neurologic consultation is usually required
Blood cultures
Urinalysis and/or cerebrospinal fluid analysis
Imaging studies
Imaging modalities used to evaluate status epilepticus may include the following:
CT scanning and/or MRI of the brain
Chest radiography for etiology
Procedures
If a central nervous system infection is suspected, consider performing a lumbar puncture (after neuroimaging to rule out potential cerebral herniation).
See Workup for more detail.
Management
Aggressive treatment is necessary for status epileptics. Clinicians should not wait for blood level results before administering a loading dose of phenytoin, regardless of whether the patient is already taking phenytoin.
Pharmacotherapy
Most patients with status epilepticus who are treated aggressively with a benzodiazepine, fosphenytoin, and/or phenobarbital experience complete cessation of their seizures. If status epilepticus does not stop, general anesthesia is indicated.
Medications used in the treatment of status epilepticus include the following:
Benzodiazepines (eg, lorazepam, diazepam, midazolam): First-line agents
Anticonvulsant agents (eg, phenytoin, fosphenytoin)
Barbiturates (eg, phenobarbital, pentobarbital)
Anesthetics (eg, propofol)
Supportive therapy
Supportive care in patients with status epilepticus includes the following:
Maintenance of vital signs
Airway, breathing, circulation (eg, hemodynamic/cardiac monitoring)
Respiratory support, with intubation and/or mechanical ventilation if necessary
Periodic neurologic assessments
Surgery
Surgical intervention for status epilepticus is a last resort and rarely performed.
Operative procedures depend on the etiology of this condition and may consist of ablating a structural abnormality, hemispherectomy, subpial resection, or placement of a vagus nerve stimulator.
See Treatment and Medication for more detail.