Practice Essentials
Herpes zoster is viral infection that occurs with reactivation of the varicella-zoster virus. It is usually a painful but self-limited dermatomal rash. Symptoms typically start with pain along the affected dermatome, which is followed in 2-3 days by a vesicular eruption. Classic physical findings include painful grouped herpetiform vesicles on an erythematous base. Treatment includes antiviral medications such as acyclovir, famciclovir, and valacyclovir given within 72 hours of symptom onset.
Reactivation of varicella-zoster virus (VZV) that has remained dormant within dorsal root ganglia, often for decades after the patient’s initial exposure to the virus in the form of varicella (chickenpox), results in herpes zoster (shingles).
While usually a self-limited rash with pain, it can be far more serious; in addition, acute cases often lead to postherpetic neuralgia (PHN) and is responsible for a significant economic burden.
See the image below.
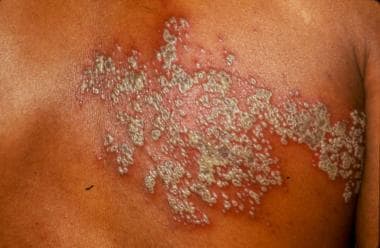
Herpes zoster, unilateral, on trunk.
See 14 Rashes You Need to Know: Common Dermatologic Diagnoses, a Critical Images slideshow, for help identifying and treating various rashes.
Signs and symptoms of herpes zoster
The clinical manifestations can be divided into the following three phases:
Preeruptive phase (preherpetic neuralgia)
Acute eruptive phase
Chronic phase (PHN)
The preeruptive phase is characterized by the following:
Sensory phenomena along 1 or more skin dermatomes, lasting 1-10 days (average, 48 hours)
Phenomena usually are noted as pain or, less commonly, itching or paresthesias
Pain may simulate headache, iritis, pleurisy, brachial neuritis, cardiac pain, appendicitis or other intra-abdominal disease, or sciatica
Other symptoms, such as malaise, myalgia, headache, photophobia, and, uncommonly, fever
The acute eruptive phase is marked by the following:
Patchy erythema, occasionally accompanied by induration, in the dermatomal area of involvement
Regional lymphadenopathy, either at this stage or subsequently
Grouped herpetiform vesicles developing on the erythematous base (the classic finding)
Cutaneous findings that typically appear unilaterally, stopping abruptly at the midline of the limit of sensory coverage of the involved dermatome
Vesicular involution: Vesicles initially are clear but eventually cloud, rupture, crust, and involute
After vesicular involution, slow resolution of the remaining erythematous plaques, typically without visible sequelae
Scarring can occur if deeper epidermal and dermal layers have been compromised by excoriation, secondary infection, or other complications
Almost all adults experience pain, typically severe
A few experience severe pain without a vesicular eruption (ie, zoster sine herpete)
Symptoms tend to resolve over 10-15 days
Complete healing of lesions may require up to a month
PHN is characterized by the following:
Persistent or recurring pain lasting 30 or more days after the acute infection or after all lesions have crusted (9-45% of all cases)
Pain usually is confined to the area of original dermatomal involvement
The pain can be severe and incapacitating
Pain can persist for weeks, months, or years
Slow resolution of pain is especially common in the elderly
PHN is observed more frequently after cases of herpes zoster ophthalmicus (HZO) and in instances of upper-body dermatomal involvement
Less common postherpetic sequelae include hyperesthesia or, more rarely, hypoesthesia or anesthesia in the area of involvement
Common features of herpes zoster ophthalmicus are as follows:
Classic symptoms and lesions of herpes zoster
Ophthalmic manifestations including conjunctivitis, scleritis, episcleritis, keratitis iridocyclitis, Argyll-Robertson pupil, glaucoma, retinitis, choroiditis, optic neuritis, optic atrophy, retrobulbar neuritis, exophthalmos, lid retraction, ptosis, and extraocular muscle palsies
Other forms include the following:
Herpes zoster of maxillary branch of cranial nerve (CN) V
Herpes zoster of mandibular branch of CN V
Herpes zoster oticus (Ramsay Hunt syndrome)
Glossopharyngeal and vagal herpes zoster
Herpes occipitocollaris (vertebral nerves C2 and C3 involvement)
Herpes zoster encephalomyelitis
Disseminated herpes zoster
Unilateral herpes zoster involving multiple dermatomes
Recurrent herpes zoster
Herpes zoster involving urinary bladder, bronchi, pleural spaces, or gastrointestinal tract
Herpes zoster with motor complications
See Clinical Presentation for more detail.
Diagnosis
Diagnosis is based primarily on the history and physical findings. In most cases, confirming the diagnosis via laboratory testing has no utility. In select patient populations, however—particularly immunocompromised patients—the presentation can be atypical and may require additional testing.
Laboratory studies for VZV include the following:
Direct fluorescent antibody (DFA) testing of vesicular fluid or a corneal lesion
Polymerase chain reaction (PCR) testing of vesicular fluid, a corneal lesion, or blood
Tzanck smear of vesicular fluid (lower sensitivity and specificity than DFA or PCR)
See Workup for more detail.
Management
Episodes of herpes zoster are generally self-limited and resolve without intervention; they tend to be more benign and mild in children than in adults.
Conservative therapy includes the following:
Nonsteroidal anti-inflammatory drugs (NSAIDs)
Wet dressings with 5% aluminum acetate (Burrow solution), applied for 30-60 minutes 4-6 times daily
Lotions (eg, calamine)
Primary medications for acute zoster–associated pain include the following:
Narcotic and nonnarcotic analgesics (both systemic and topical)
Neuroactive agents (eg, tricyclic antidepressants [TCAs])
Anticonvulsant agents
Steroid treatment is traditional but controversial. Typically, a substantial dose (eg, 40-60 mg of oral prednisone every morning) typically is administered as early as possible in the course of the disease and is continued for 1 week, followed by a rapid taper over 1-2 weeks.
Antiviral therapy may decrease the length of time for new vesicle formation, the number of days to attain complete crusting, and the days of acute discomfort. Usually, the earlier antiviral medications are started, the more effective they are in shortening the duration of zoster and in preventing or decreasing the severity of PHN. Ideally, therapy should be initiated within 72 hours of symptom onset.
Oral treatment with the following has been found beneficial:
Acyclovir
Famciclovir
Valacyclovir
Hospital admission should be considered for patients with any of the following:
Severe symptoms
Immunosuppression
Atypical presentations (eg, myelitis)
Involvement of more than 2 dermatomes
Significant facial bacterial superinfection
Disseminated herpes zoster
Ophthalmic involvement
Meningoencephalopathic involvement
Prevention
The routine use of the live attenuated varicella vaccine has led to a remarkable reduction in the incidence of primary varicella infection. Prevention or attenuation is particularly desirable in older patients because zoster is more frequent and is associated with more complications in older populations and because declining cell-mediated immunity in older age groups is associated with an increased risk of zoster.
Vaccines available in the United States include the following:
Varivax for children
Shingrix for older adults
The CDC recommends administration of varicella-zoster immune globulin to prevent or modify clinical illness in persons with exposure to varicella or herpes zoster who are susceptible or immunocompromised.
Prompt treatment of acute zoster and its associated pain (eg, with antiviral therapy) can prevent the development of PHN. Once PHN has developed, various treatments are available, including the following:
Neuroactive agents (eg, TCAs)
Anticonvulsant agents (eg, gabapentin,
pregabalin)
Narcotic and nonnarcotic analgesics, both systemic (eg, opioids) and topical
See Treatment and Medication for more detail.